Nominations are now open for the 3D Printing Industry Awards 2023. Who are the leaders in 3D printing? Find out on November 30th when the winners across twenty categories will be announced during a London-based live awards ceremony.
Researchers from Queen’s University Belfast have developed personalized 4D printed implants to manage and treat breast cancer. This is said to be the first time that 4D printing has been used to produce breast cancer implants.
4D printing is essentially the production of dynamic 3D printed objects out of so-called “smart materials” that can change their characteristics and morphology. These changes can be programmed and accurately predicted, and are controlled by external stimuli such as variation in pH, temperature, humidity, light, or magnetic fields.
Using this technology, the research team produced multipurpose breast implants that can be programmed to change size to better fit into a patient’s tissue cavity. This allows for greater personalization and improved aesthetic outcomes. Moreover, the 4D printed implants can also release chemotherapy drugs exactly where they are needed, protecting the patient from the return of cancer cells in the affected area.
“By making, for the first time, these 4D printed implants, the breast cavity after surgery can be covered with an implant that mimics the elasticity of the breast and provides better management of the breast cancer by releasing a chemotherapeutic drug that will “keep away” the return of the tumor,” commented Professor Dimitrios Lamprou, lead on the project and Chair of Biofabrication and Advanced Manufacturing from the School of Pharmacy at Queen’s University Belfast.
The research paper has been published in the journal Science Direct.

Treating breast cancer with 4D printing
The second most common cancer in the world, more than 2.3 million breast cancer cases occur each year, with around 30% of those affected dying from the disease.
Breast-conserving surgery is the primary strategy for treating early-stage breast cancer, however local cancer recurrence and breast tissue loss are commonly associated with this treatment method. Additionally, the use of radiotherapy and systemic therapy, while increasing the patient’s survival chances, results in longer treatment durations and unpleasant side effects. The Queen’s University team claim to have developed an appealing alternative to these methods.
Given the heterogeneity between individuals and tumors, the researchers argue that “a patient-centered approach is fundamental” to treating breast cancer. This is where additive manufacturing comes in. The researchers argue that 4D printing presents an opportunity to improve the management of breast cancer through the development of “smart implants.”
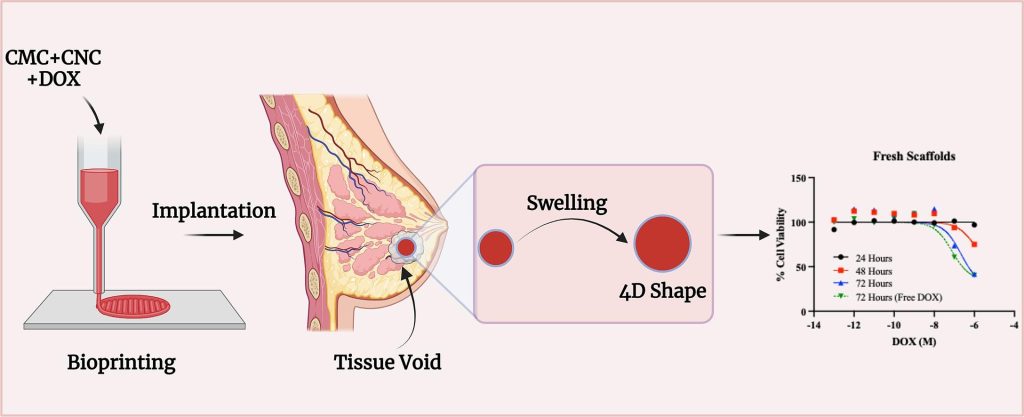
Leveraging the Tinkercad 3D CAD design tool and a Cellink Bio X 3D bioprinter, the research team manufactured breast implants with a blend of carboxymethyl cellulose sodium salt (CMC) and cellulose nanocrystals (CNC). The implants were also loaded with doxorubicin (DOX), a common chemotherapeutic drug, which could then be delivered in a concentrated and targeted manner to reduce the probability of the cancer returning.
“Chemotherapy plays a crucial role in the treatment of breast cancer, but it is associated with harsh side effects,” explained Dr Niamh Buckley, Reader from the School of Pharmacy and responsible for the in vitro evaluation of the implants. “The use of technology such as this, which allows a concentrated delivery of the drug just to where it is needed, can help make treatment more effective and kinder.”
The researchers also noted that magnetic resonance imaging (MRI) or computerized axial tomography (CAT) scans could be used to customize the implant according to the patient’s needs. Moreover, once implanted, the 4D printed “smart device” can expand to better conform to the patient’s body. This change in size and shape occurs as a response to the patient’s interstitial fluids (the fluids that fill the gaps between cells), providing an extra level of customization based on the patient’s profile.
Thanks to their small size, these breast implants are also affordable and easy to manufacture. As such, they can be prepared in hospitals for direct and personalized treatment, reducing costs and providing better options for patients.
3D bioprinting and cancer treatment
This research reflects a growing trend of employing additive manufacturing technology to aid cancer patients both during and after treatment. For instance, last year it was announced that researchers at Laval University in Canada had developed a novel 3D printed hydrogel that could be used to treat cervical cancer.
The gel, composed of a thermosensitive polymer mixed with gold nanoparticles, was designed to be applied locally to the vagina where it can then directly carry drugs to the cervixes of female cancer patients. What’s more, the research team noted that, with further R&D, scan data could be used to personalize their hydrogel to the anatomies of specific patients.
Elsewhere, leading US-based additive manufacturing company 3D Systems recently announced plans for a Regenerative Tissue Program (RPT) which aims to develop and commercialize bioprinted human tissue. The first RPT product under development relates to patient-specific regenerative breast tissue (RBT).
This tissue meets a growing demand for post-breast cancer regenerative breast reconstruction. 3D Systems claims that by combining 3D modeling and 3D bioprinting with its Virtual Surgical Planning (VSP) system, it can design and produce bio-integrative scaffolds that match the patient’s anatomy and physiology.
Subscribe to the 3D Printing Industry newsletter to keep up to date with the latest 3D printing news. You can also follow us on Twitter, like our Facebook page, and subscribe to the 3D Printing Industry Youtube channel to access more exclusive content.
Are you interested in working in the additive manufacturing industry? Visit 3D Printing Jobs to view a selection of available roles and kickstart your career.
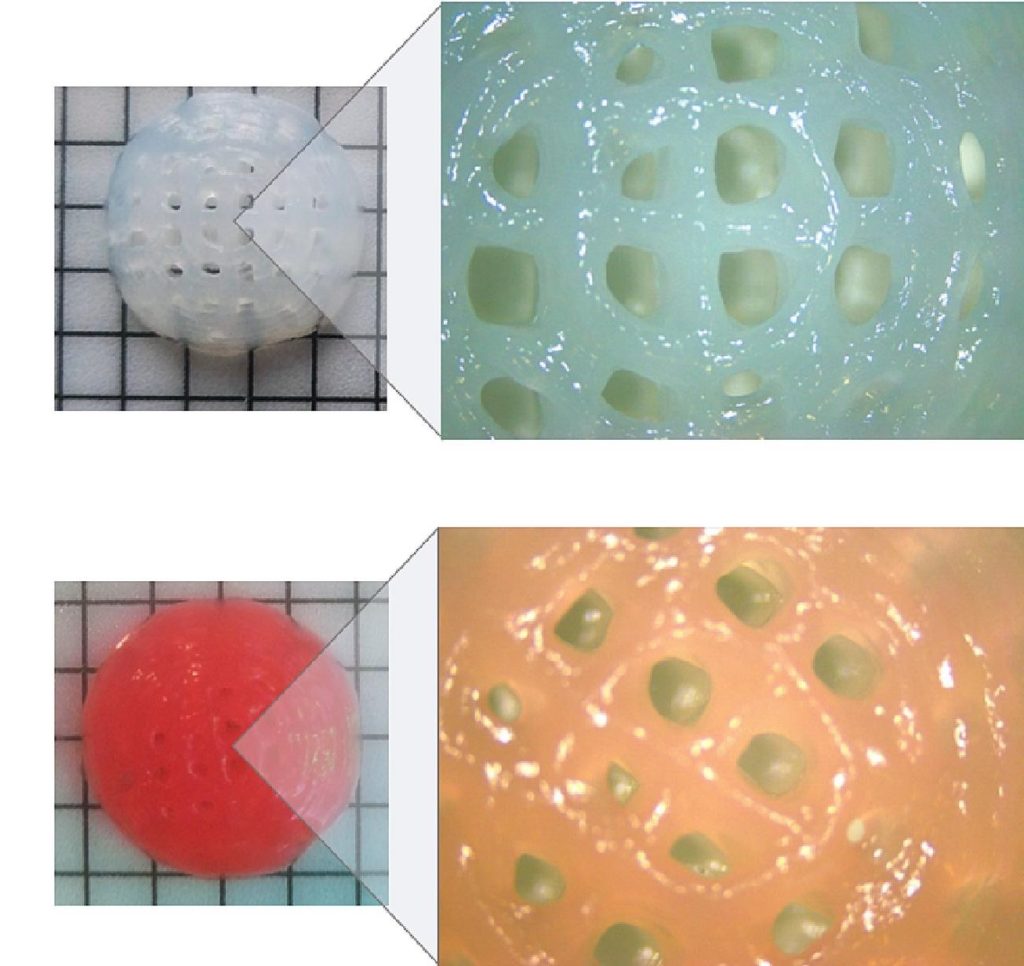
Featured image shows a blank implant (top) and a DOX-loaded implant. Image via Queen’s University Belfast.
منبع: https://3dprintingindustry.com/news/researchers-4d-print-personalized-smart-implants-to-treat-breast-cancer-224307/?utm_source=rss&utm_medium=rss&utm_campaign=researchers-4d-print-personalized-smart-implants-to-treat-breast-cancer
